Insurers can use the data collected by these devices to develop products and services that are geared to their customers’ individual needs. They can also offer incentives for good behavior, such as discounts on auto insurance premiums for drivers who regularly stay within the speed limit, or rebates for life and health insurance customers who exercise regularly. Because the FTC does not necessarily perform a formal econometric calculation of the hypothetical monopolist test during investigations, FTC staff generally seeks qualitative evidence that mimics the test.
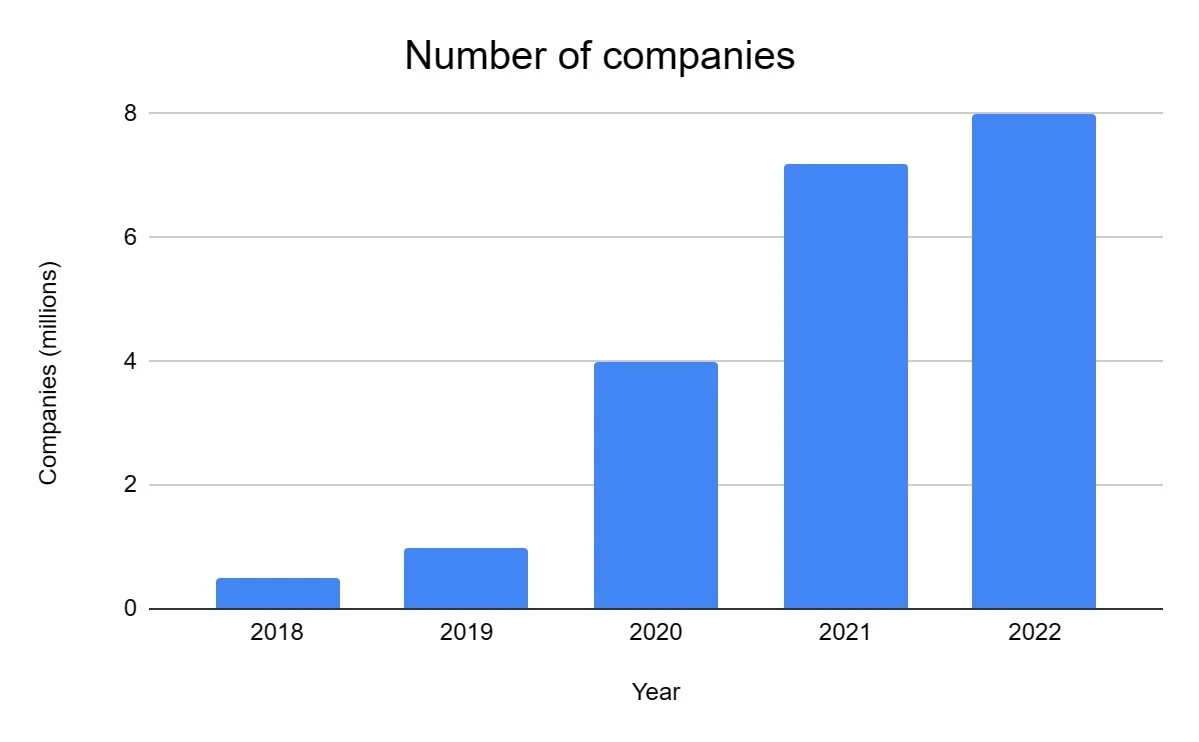
Zhong An, the online insurer launched in 2013 and backed by Ping An, Tencent and Alibaba, is a vivid example of the growing appeal of digital insurance in China. In 2018, the company served more than 400 million customers and sold more than 6 billion policies—although, granted, many of those policies involved short-term coverage for e-commerce activities. For connectivity, smart insurers are taking a cue from their own customers, many of whom already use connected devices to monitor their cars, their homes and their health. Worldwide, 39% of insurance customers surveyed by Bain & Company currently use at least one connected device, and about 72% expect to use one in the future.
Payers reducing the need for prior authorizations – what healthcare organizations need to know
Geographic market definition is often one of the most difficult and contested issues in a provider-merger investigation and litigation. The FTC typically defines the geographic market in provider mergers as a relatively narrow local market. For example, in recent enforcement actions, the FTC has defined geographic markets as narrowly as a county or portions of two counties, and as broadly as multi-county areas around merging hospitals. The analysis and relevant evidence https://www.globalcloudteam.com/ in geographic market definition are essentially the same in hospital, outpatient, and physician mergers. In terms of qualitative evidence, the FTC evaluates testimony and documents from the merging providers and area insurers, rival hospitals, and employers about several factors in defining the geographic market. The Council for Affordable Quality Healthcare (CAQH) is a not-for-profit organization formed by some of the nation’s top health insurance companies.
The same private insurance companies will contract with the state to cover care for Medicaid patients and accept financial risk. Many patients have been added over the last several years to managed Medicaid plans via the Patient Protection and Affordable Care Act (ACA). The sixth step to building relationships with healthcare stakeholders is to evaluate and improve. healthcare software development This means assessing the quality, effectiveness, and impact of your relationships and finding ways to enhance them. Evaluation and improvement are essential for building rapport, mutual understanding, and collaboration with healthcare stakeholders. The second step to building relationships with healthcare stakeholders is to establish trust and credibility.
The 5 provider strategies to improve profit margins
In this framework, the relative bargaining leverage of the provider and the insurer largely determines the outcome of that price negotiation. The more leverage a provider has, the more likely that it can negotiate for higher rates; conversely, the more leverage the insurer has, the more likely that it can resist rate increases. The FTC is concerned about provider mergers that substantially lessen competition because that may provide the merged firm with enhanced bargaining leverage and enable it to extract higher prices. Many healthcare provider mergers—either due to their relatively small size or the structure of the transaction—do not trigger an HSR-filing requirement. Importantly, however, the antitrust agencies can still investigate—and challenge—a transaction that does not require an HSR filing.
To help clear the confusion, this article details the basics of provider credentialing and offers recommendations on fulfilling the responsibilities as efficiently and effectively as possible. Furthermore, the software can add actionable alerts, creating flags when payers change their requirements. For example, the Prior Authorization Knowledgebase, a proprietary repository for more than 160 national payers and their pre-certification rules, allows quick check functionality to see if a procedure requires appropriate use criteria adherence. Users can create service work queues when CMS requires adherence to Appropriate Use Criteria (AUC). Two supporting tools to aid these processes include the Medical Necessity tool, which validates clinical orders against CMS and private payer rules for fewer denials, and Claims Scrubber, which helps healthcare organizations prevent denials by improving claims accuracy.
Using Technology to Streamline Prior Authorizations
We also assessed how the product ownership changed in the past year, i.e., how many customers switched to competitors vs. how many new customers were acquired. We analyzed this at an overall market level as well as at a provider level for all products or a business line (P&C or life) or at a product level (auto or home or life protection or life savings). When developing digital muscles, insurers tend to lag behind other industries and their own customers. Many consumers now opt for digital channels from the moment they start thinking about buying insurance.
You may be wondering what power you really have to influence the suits in the fancy building. Healthcare finance content, event info and membership offers delivered to your inbox. The trend shifted in Q3 2020, when volumes of elective procedures began to rebound. While operating cash-flow margins improved for all tiers of organizations that were analyzed, margins were slightly higher for organizations with no more than 20% of revenue tied up in PSHPs and capitation.
Accelerating Change in Medical Education Award
Today, better health requires reducing the complexities of the healthcare paradigm. Experian Health offers provider organizations improved options for delivering care with robust technological solutions that improve the lives of clinicians, staff, and patients. We specialize in offering digital tools to improve every stage of the patient journey.
- So even if a transaction is not reportable under the HSR Act, the FTC may still hear about and investigate the transaction if it raises competitive concerns, which might be more disruptive post-closing.
- This involves creating a “secret” that is used when exchanging the authorization code to obtain an access token.
- Telehealth and remote patient monitoring will become an essential, cost-effective and reliable means to expand capacity in a health system marked by significant and persistent specialty shortages and geographic disparities.
- If the member declines to share information that your application needs, you may display a message explaining why that information is needed and request re-authorization or handle the collection of that information elsewhere within your application.
- Davis-Green, the Louisiana healthcare consultant, says that during her work in credentialing organizations, she made sure to become friendly with people at licensing and similar agencies, who can help get information more quickly.
- Dr. A. Mark Fendrick, director of the University of Michigan’s Center for Value-Based Insurance Design (V-BID) in Ann Arbor, Michigan, said this rule moves the country’s healthcare system toward greater price transparency.
There is a shimmer of hope as some insurers are retracting prior authorization prerequisites for certain conditions and procedures. However, this move might produce more complexities, given the distinct protocols of each payer. The traditional manual handling of prior authorizations by most providers leaves ample room for errors amidst these changes. Experian Health’s electronic prior authorization software can expedite and streamline pre-certification workflows, keeping providers updated with the ever-evolving payer requirements. Under original Medicare, participants can purchase Medigap coverage to pay some or all of their coinsurance costs. These plans, also known as Medicare supplement insurance plans, are issued by private insurers and regulated by the states.
Medical education leadership opportunities
In addition to the inpatient GAC product market, the FTC may also allege a separate inpatient market for individual hospitals’ services where the competitive conditions for a service differ meaningfully from the overall inpatient GAC market. You might see this where there are fewer competitors offering that individual service and the merging parties’ market share in that service is meaningfully higher than in the inpatient GAC market. Therefore, you should assess whether there are any overlapping inpatient services where the parties’ combined market share, and where market concentration, is significantly higher.

A network is a group of doctors and hospitals that accept a certain health insurance plan. It is critical to get to the decision-maker on important issues to avoid wasting time and becoming frustrated. This requires learning about the payer.8 For example, if your goal is to reduce the time spent on imaging authorizations, your contact will be one of the medical directors. The provider representative is unlikely to be helpful in resolving this problem. If you are spending a lot of time arranging home infusion, then you need to find the Director of Care Management. If you are looking for better reimbursement, you need someone in contracting who can move off a standard fee schedule.
Comentarios recientes